By Josefien van Olmen, Tanja Stjepanovič, Srean Chhim, Daniel Boateng, Katrien Danhieux and Monika Martens
One year ago, in February 2020, the SCUBY team convened for its second Consortium Meeting in Siem Reap, Cambodia. We had the beauty of the place practically to ourselves, since the usual thousands of Chinese tourists were confined to their country in COVID lock-down. The Cambodian hosts were extremely welcoming and we cherish the best memories to our gathering and the environment. COVID shadows were looming, but the SCUBY team was confident to continue their ambitious plans to improve and scale-up diabetes care in each country.
Very soon after our return to work, we faced the growing COVID reality. Priorities changed, chronic care was pushed aside to free capacity and space for people with COVID-suspect symptoms. Patients, health care workers, hospital managers, policymakers. All of us in society had to follow, bound by restrictions, lockdowns and facemasks.
It also affected our SCUBY work and plans. We had to postpone field work, we had to change interviews to Zoom-mode, we could not reach stakeholders to develop a joint scale-up agenda. We realised that this is real-life research and that we needed to adapt. Read below how each partner did.

Slovenia, by Tanja Stjepanovič
In Slovenia, the first infection with the new coronavirus was confirmed on March 4, 2020. Currently, we are dealing with the second wave of epidemics, which is hitting us much harder than the first one. The epidemiological situation is being monitored with increased testing and depending on the number of people infected, measures are being taken and adapted to contain the spread of the new coronavirus in our country. As we are experiencing a rapid and exponential spread in the population, intensified measures follow, which in certain cases affect our work and require changes in the implementation plans.
Work on the formative work package was completed on time and successfully without delays. Meanwhile, work on the financial analysis and on monitoring was hampered by the workload of medical staff engaged in epidemiological tasks. It was a challenge to encourage them to participate in the research. Now we are deep in the scale-up work and evaluation planning, which are even more affected by the current health crisis. So the situation we are in now affects us all. It requires a higher level of resourcefulness, flexibility and collaboration. Therefore, we are struggling hard to stay within the planned activities and deadlines.

Cambodia, by Srean Chhim
Cambodia detected the first case of COVID-19 on 27 February 2020. Cambodia did not experience community transmission until 28 November 2020. The community transmission, however, was contained within two months. Cambodia’s achievement in containing the spread of the virus was possibly from the travel restriction, flight disconnection, closure of all schools, and closure of all gathering sites to reduce transmission. These policies impacted our work along the entire scope of the project... The work on costing and financing was affected by the population-based survey’s delay, including the demand-side cost of using diabetes type-2 (T2D) and hypertension (HTN) service. The population-based survey was however conducted, three months later than its original plan. Second, the population-based survey’s delay also impacted the construction of a cascade of care to monitor the outcomes of care. Another element, the NCD monitoring system evaluation, was also impacted by staff’s unavailability. Third, the roadmap development and implementation heavily rely on sufficient evidence to be generated to inform policies. So the evidence delay in turn impacts the scale-up roadmap, and ultimately, the evaluation of scale-up strategies and roadmap. In summary, the COVID-19 situation in Cambodia has delayed the entire process from population-based survey to evaluation.
The Netherlands, by Daniel Boateng
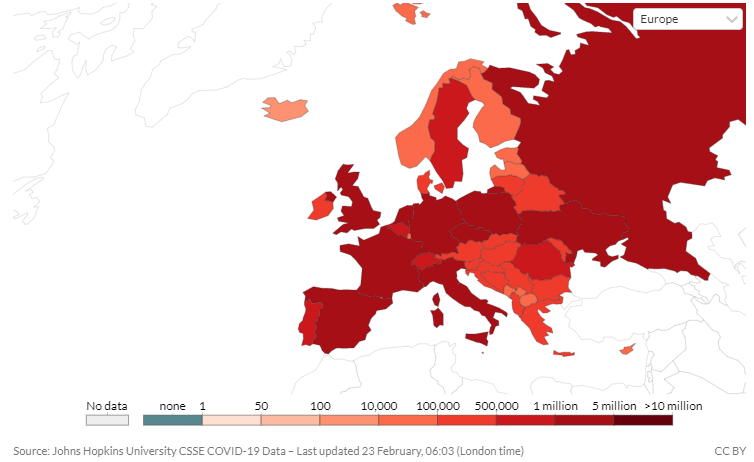
The Netherlands reported its first confirmed case of coronavirus on the 27th of February, 2020. Almost a year on, the country is hit hard by a second and third wave of the pandemic. This has to some extent affected the roadmap and evaluation work of the SCUBY project. Although the Netherlands is not an implementing country, the mandate to evaluate the impact and process evaluations is dependent on the other work packages and fieldwork in the implementing countries. We are however making the best out of the moment, collaborating with implementing countries and other work packages to develop protocols and plan for the impact and process evaluations. As put forward by Socrates, "The secret of change is to focus all of your energy, not on fighting the old, but on building the new.” We are adapting to the new way of work, and remain resolute in the hope of reaching our goal.
Belgium, by Katrien Danhieux
Belgium was one of the countries hit hardest in the first wave. While the health care workers within our team helped in patient triage, testing and care we also took this opportunity to investigate this special and interesting situation. As interviews with providers about the implementation of integrated care were carried on and switched to online video interviews we added a few questions on how the crisis impacted the care for patients with chronic diseases in primary care. It seemed that such a crisis emphasizes strongly the deficiencies of the system. We wrote it down on a paper.

The cross country lessons, by Monika Martens
We all have our own context- and health system-specific challenges. COVID-19 has been a common denominator to challenge the SCUBY project as a whole. Emergency response strategies to the epidemic have been prioritised in our different country settings - whereas global attention has shifted towards this crisis (and tackling this crisis) over the past year -, putting our project’s objectives of scaling and evaluating chronic care implementation lower on the agenda of policy-makers. In these challenging times, it’s important to realise that not just the outcomes of our project that will be affected in one way or another (positively or negatively; likely more health inequity, yet more attention to health systems functioning, financing and digital health monitoring?), but also our collaborators have been affected greatly. Here the question arises: will we be able to build back better? Is this a threat to current (or long-ongoing) efforts or an opportunity for the renewed commitment? As co-creating strategies and solutions for care integration via policy dialogue is at the core of the project, we should be aware of the shift in mindsets and priorities of stakeholders and policy-makers and focused on improving access for the vulnerable - hardest hit by COVID-19.
It’s hard to think of something that remains unaffected: our minds, our work, our daily lives... In spite of all this, our resolve is strong to continue to go into dialogue with each other in this new normal, and to find new solutions in new ways.


Comments